Gum Disease Treatment
- Home
- Gum Disease Treatment
At Acts Dental Perth, we care for your oral health. Our dentists specialise in gum disease treatment to help you maintain a pretty and healthy smile.

What is gum disease and how is the treatment for it?
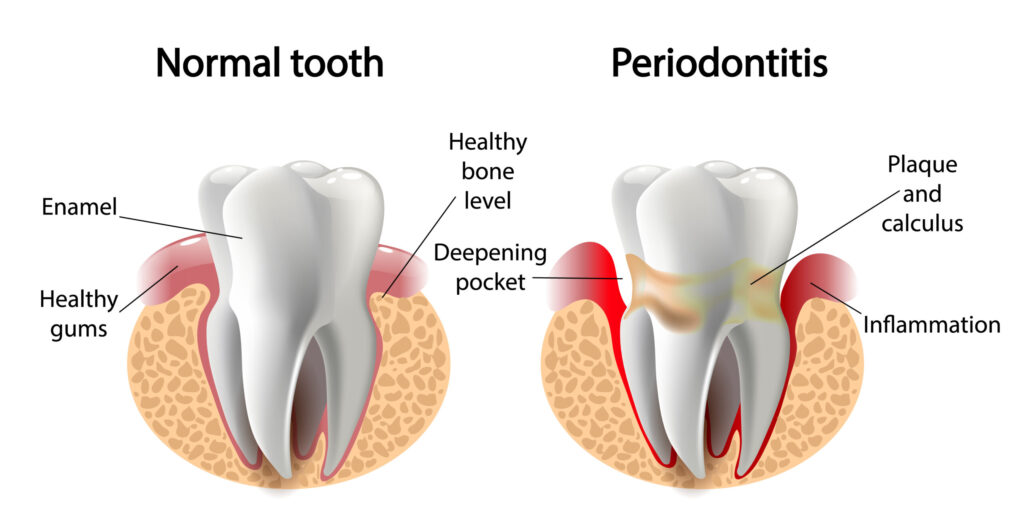
Gum disease , also known as periodontal disease, is a condition that can affect the tissues surrounding and supporting the teeth. One of the main causes of gum disease is the bacteria found in plaque, a sticky film that forms on the teeth. If dental plaque is not thoroughly and properly removed through brushing and flossing, it can turn into a hard substance called tartar or calculus. Buildup plaque can lead to poor oral health and increase the risk of gum disease.
Gingivitis is a mild form of gum disease that is typically reversible if you practice good oral hygiene. However, if gingivitis is not addressed and is left untreated, it can progress to periodontitis or gum disease abscess. Periodontitis, also known as gum disease abscess, is a more severe form of gum disease that can destroy the bone that supports your teeth and even cause tooth loss if not treated.
If you need an urgent visit to the dentist, call Acts Dental Perth straight away. Our emergency dentists in Perth are ready to help with your last-minute call.
What Causes Gum Disease?
Several risk factors can lead to gum disease and make it worse over time. One of the biggest factors is poor oral hygiene. If you don’t brush and floss properly, plaque can build up on your teeth and along your gum line, increasing the risk of gum disease. A number of other factors can also contribute to the development of gum disease, including smoking, hormonal changes, genetics, the use of certain medications, and even underlying systemic diseases.
Signs and Symptoms of Gum Disease
Knowing the symptoms of gum disease can help you act quickly and get the right gum disease treatment. Below are some of the most common warning signs to look out for.
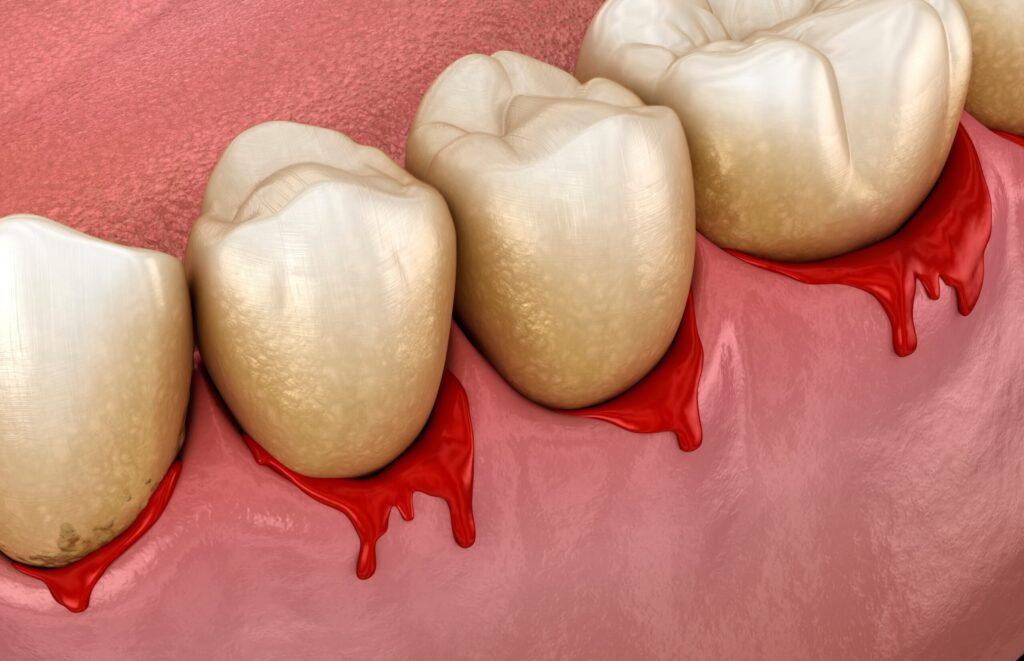
Swollen or Bleeding Gums
If your gums are swollen or bleed easily, it could be an early sign of gum disease. When your gums get irritated and inflamed, they may look red, swollen, or sore. You may also notice some bleeding when you brush or floss.
Bad Breath
Constant bad breath could also be a warning sign that you might need gum disease treatment. The buildup of harmful bacteria in your mouth can lead to an unpleasant smell.
Sensitive Teeth
If you feel pain or discomfort when eating or drinking something hot, cold, sweet, or acidic, it may be a sign of gum disease. When gums start to recede, they can expose the sensitive roots of your teeth, making them more sensitive.
Receding Gums
Gum recession happens when the gums pull away from the teeth, exposing the roots. This can be a sign of advanced gum disease. When the gums recede, gaps can form between the teeth and gums, making it easy for bacteria to collect and cause even more damage. In those cases, we highly recommend a visit to the dentist.
Loose Teeth
In the advanced stages of gum disease, the bone and tissues that support your teeth can get damaged. This can lead to loose teeth or changes in how your teeth align. If you notice any of your teeth feeling loose or shifting around, it could be a sign of serious gum disease. It’s important to see your dentist right away to seek gum disease treatment and avoid losing any teeth.
Importance of Early Detection and Gum Disease Treatment
It is crucial to treat gum disease in its early stages before it can result in tooth loss and other oral health problems. Gum disease treatment usually means getting professional dental care, like deep cleaning to get rid of plaque and tartar, along with keeping up good brushing and flossing habits at home.
Diagnosing Periodontal Disease
To diagnose gum disease, your dentist will do a dental exam, ask about your medical history, and use a special tool called a periodontal probe to check how deep the pockets are around your teeth. This helps them see how serious the gum disease is. They’ll look for signs like gum swelling, loose teeth, and plaque buildup. Your medical history also helps them understand what may be causing the issue. But once diagnosed, how can you treat gum disease effectively?
Nonsurgical Treatments
The first step dentists take when treating gum disease is typically nonsurgical methods. These nonsurgical approaches focus on removing plaque, tartar, and harmful bacteria from your teeth and gums, which helps them heal and prevent further damage.
Scaling and Root Planing
Scaling and root planing is a deep cleaning procedure used to clean along the gum line and the surfaces of your teeth. This non-surgical procedure is usually recommended if your gum pockets are deeper than usual, which can mean you have gum disease.
During scaling, your dentist or dental hygienist uses special tools to remove plaque and hardened tartar from your teeth and under the gums to eliminate the bacteria that cause gum inflammation and infection.
Root planing smooths out the rough spots on the roots of your teeth. It helps remove any remaining bacteria and makes it easier for your gums to reattach, help them heal, and stop the gum disease from getting worse.
Antibiotics for Gum Infections
Sometimes, antibiotics are prescribed to help treat gum infections as an alternate gum disease treatment. They help control bacteria growth and reduce inflammation, which helps with the healing process.
Your dentist may prescribe oral antibiotics for a short time to address acute gum infections. Topical antibiotics can also be applied directly to the infected periodontal pockets. These antibiotics focus on the bacteria in that area, help it heal, and lower the risks of further gum disease infection.
Remember that antibiotics are usually used along with other treatments and good oral care. Your dentist will decide the best type of antibiotics for you, depending on how serious the infection is and your overall dental health.
Dental Cleaning
Regular dental cleanings are necessary for keeping your teeth and gums healthy, especially if you have gum disease. A dental hygienist usually performs these cleanings, and they work together with your brushing and flossing at home to improve your oral health.
Surgical Treatment for gum disease
If nonsurgical treatments are not effective or enough, your dentist may consider surgical approaches. Surgical procedures are considered to help fix specific issues such as tooth root exposure, bone loss, or soft tissue deficiencies.
Flap Surgery
Flap surgery, or pocket reduction surgery, is a surgical procedure to treat periodontitis. During this procedure, the dentist makes small cuts in your gums to lift them back, which helps them reach the roots of your teeth and the bone underneath.
Then, the dentist cleans the tooth root and removes any infected or damaged tissue. Sometimes, dentists may also reshape the bone to eliminate irregularities and fix any uneven areas. After the cleaning and reshaping steps are finished, the dentist repositions and sutures the gums. This helps make the pockets smaller, so it’s easier for you to keep your mouth clean and prevent further damage.
Bone Grafts
If periodontitis has caused severe damage to your gums, your dentist may decide that you need bone grafts. The goal of bone grafting is to help grow back the lost bone so it can support your teeth and keep your mouth healthy. During the procedure, the dentist will place donated bone, synthetic bone, or other graft materials in the area where the bone is missing to help the bone grow back.
Gum Tissue Graft
You may need a surgical procedure called “soft tissue grafts” if you have gum recession. This surgical procedure is used to improve the appearance and health of the gum line that has been affected by gum recession. During this procedure, the dentist or periodontist takes a small piece of gum tissue from another part of your mouth or uses donated gum tissue. The dentist then places the graft over the receding gums to cover the exposed tooth roots. This helps protect the roots, reduce sensitivity, and stop the gums from further recession.
Guided Tissue Regeneration (GTR)
For patients with lost bone and periodontal tissues, a surgical procedure called “guided tissue regeneration” may be the viable option. If you have significant bone loss, your dentist may decide to perform GTR for you. The procedure helps regenerate the supporting structures around your teeth. During the treatment, your dentist will place a barrier membrane between the gum tissues and the tooth root to prevent unwanted tissue from growing into the area. This will allow the bone and gum tissue to grow back properly.
How to Prevent Gum Disease
Preventative dental care is an important step in taking care of your oral health. Following these steps can help prevent gum disease and keep your teeth healthy.
Practice Proper Dental Hygiene: Brush your teeth at least twice daily and use fluoride toothpaste. Fluoride strengthens the tooth enamel and protects against tooth decay. Use a soft toothbrush and brush all surfaces of your teeth and along the gum line. Change your toothbrush every three to four months or sooner if it starts to look worn out.
Floss Daily: Flossing removes dental plaque and food particles stuck between teeth and the gum line. It is an essential part of oral hygiene because it helps prevent the buildup of bacteria that can lead to gingivitis. Use a gentle, back-and-forth motion to clean between each tooth. If traditional flossing is challenging, you can use floss picks or interdental brushes.
Visit Your Dentist Regularly: Regular dental check-ups and cleanings are crucial for maintaining good oral health and preventing oral diseases. It is recommended to visit your dentist at least once every six months. During regular visits, your dentist can spot the early signs of gum disease and provide appropriate treatment or tips to prevent it.
Maintain a Healthy Lifestyle:
A healthy lifestyle can help you maintain your oral health. Try to stay away from tobacco because it significantly increases your risk of gum disease. It is also important to cut down on sugary and acidic foods and drinks since they can cause cavities and other dental issues. To enjoy optimal oral health, it’s better to go for a balanced diet with lots of fruits, veggies, whole grains, and lean proteins.
Manage Medical Conditions:
If you have conditions like diabetes, you need to be extra careful with your gums because they may increase your risk of gum disease. It’s really important to keep these conditions under control and stay in touch with both your doctor and your dentist.
Be Aware of Warning Signs: Pay attention to early signs of gum disease because addressing gum disease at its early stages can make a big difference in your oral health. If your gums look red, swollen, feel sore, or bleed when you brush or floss, or if you have bad breath or notice your gums pulling away from your teeth, those could be signs of gum disease, which should take you to the dentist as soon as possible.
We’re here to help
Please remember that gum disease can silently progress and impact your smile and overall well-being. That’s why early treatment and prevention and finding the best dentist for gum disease in Perth are important to keeping your gums and teeth healthy for life. At Acts Dental Perth, we provide our patients with the care and attention they need to improve their dental health and enjoy a healthy smile. Whether it’s a professional tooth cleaning or advanced gum disease treatment, we’re here to support your oral health. Don’t let gum disease get worse—give us a call at (08) 9474 5083 and schedule your appointment today
