Root Canal Treatment
- Home
- Root Canal Treatment
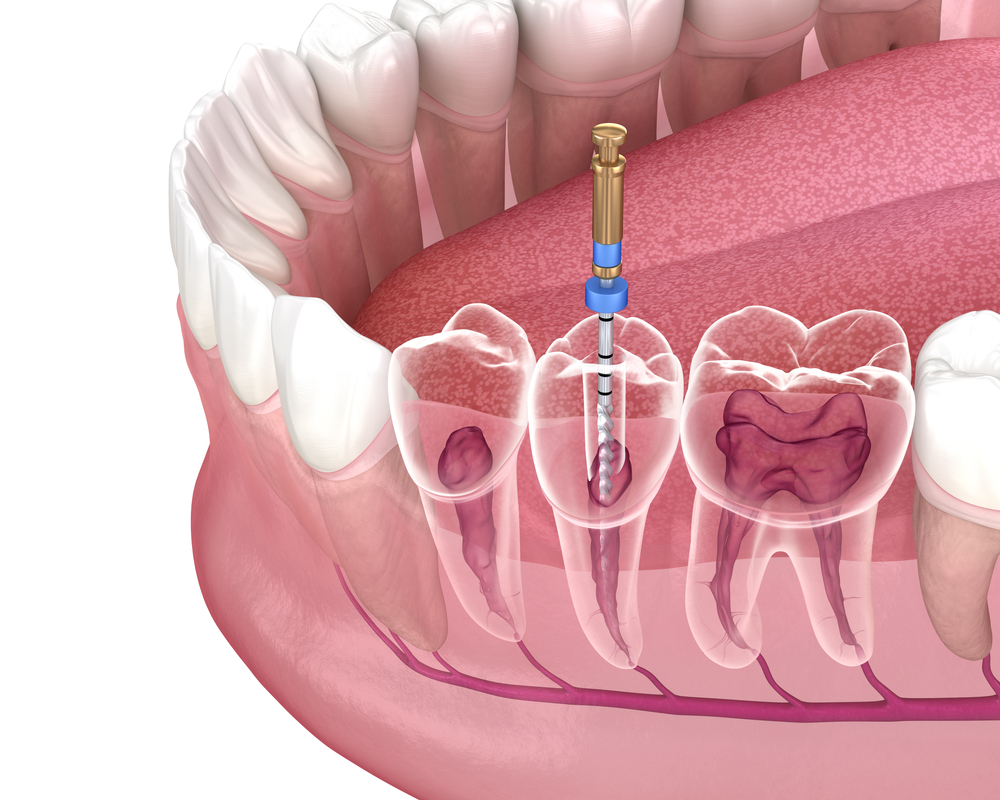
What is Root Canal Treatment?
Root canal treatment Perth, or "endodontic treatment", is a dental procedure to save a decayed tooth that is severely infected or damaged at the pulp level.
The dental pulp is the innermost part of the tooth, containing nerves, blood vessels, and connective tissue.
Root canal treatment is necessary when the dental pulp becomes infected or inflamed due to deep decay, repeated dental procedures, cracks, or trauma.
During a root canal procedure, the dentist or endodontist (a specialist in this field) removes the inflamed or infected pulp, ensuring a thorough cleaning and disinfection of the root canals. These are then sealed with a biocompatible material known as gutta-percha. By doing so, it not only addresses the infection but alleviates pain, retains the tooth’s structural integrity, and bolsters oral health.
Opting for a root canal treatment, especially by experienced Perth dentists, is advantageous over tooth extraction. It ensures the natural tooth remains intact, preserving optimal biting and chewing functionality and warding off potential shifts of adjacent teeth. Following this treatment, it’s customary to fit a dental crown to the treated tooth, reinforcing its strength and protection.
In essence, root canal treatment stands as a prevalent and proficient method to rescue a jeopardized tooth that might otherwise warrant removal.
Purpose of Root Canal Therapy
The primary purpose of root canal therapy is to save a tooth affected by deep decay, infection, or damage to the dental pulp. The tooth can be preserved, and its functionality can be restored by root canal treatment.
Here are the key purposes of root canal therapy:
Elimination of Infection: Root canal treatment removes the inflamed or infected pulp tissue from the tooth. That helps eliminate bacteria and prevent infection from spreading to surrounding tissues.
Pain Relief: Infected or inflamed pulp tissue can cause severe pain and discomfort. Root canal therapy aims to alleviate pain by removing the source of the infection and reducing inflammation.
Preservation of Natural Tooth: Saving the natural tooth is generally the preferred option over extraction whenever possible. Root canal treatment allows for preserving the tooth’s structure, function, and appearance.
Restoration of Chewing Ability: A tooth that has undergone a root canal or endodontic therapy can continue to function properly for biting and chewing, contributing to overall oral health and maintaining a balanced bite.
Prevention of Tooth Loss: By treating the infected tooth with root canal procedures, the need for extraction is avoided. It helps maintain the natural alignment of the teeth and prevent potential issues that may arise from tooth loss, such as shifting the surrounding teeth or jawbone deterioration.
Signs and Symptoms of Root Canal Infection
When a tooth is experiencing problems that may require root canal therapy, there are several signs and symptoms to watch out for. These indications suggest the tooth’s dental pulp may be infected or damaged.
Here are some common signs and symptoms that may indicate root canal issues:
Persistent Tooth Pain: Continuous or severe tooth pain, especially when biting or applying pressure, can indicate the need for a root canal. The pain may linger even after the stimulus is removed.
Sensitivity to Hot and Cold: Increased sensitivity to hot or cold temperatures, which lingers even after the temperature stimulus is gone, can indicate pulp inflammation or infection.
Gum Swelling and Tenderness: Swelling and tenderness in the gums surrounding a specific tooth may indicate an underlying root canal issue. The affected area might appear red or swollen.
Prolonged Sensitivity to Touch: If a tooth becomes sensitive to touch or pressure, even without any temperature changes, it could suggest a problem with the tooth pulp.
Discolouration of the Tooth: A tooth that has undergone changes in colour, becoming darker or greyish, might indicate internal damage to the pulp.
Presence of Pus or Abscess: The development of a pimple-like bump on the gum, accompanied by facial swelling, discharge of pus, or a bad taste in the mouth, may indicate an infection that requires root canal treatment.
Tenderness or Swelling in the Nearby Lymph Nodes: In some cases, an infected tooth can cause swelling or tenderness in the lymph nodes located in the neck or jaw area. When a tooth infection spreads to the surrounding tissue, the body’s immune response may cause the lymph nodes to become reactive, resulting in localized tenderness or swelling.
It’s important to note that these signs and symptoms are not exclusive to root canal issues and may also be associated with other dental conditions.
If you are experiencing any of these symptoms, it is recommended to consult with a specialist endodontist for a proper diagnosis and appropriate treatment.
Factors Leading to Root Canal Problems
Several factors can contribute to the development of root canal problems. These factors can increase the likelihood of infection or damage to the tooth pulp, necessitating root canal treatment.
Here are some key factors leading to root canal problems:
Dental Decay: Untreated tooth decay is one of the primary causes of root canal issues. When a cavity is left untreated, it progresses deeper into the tooth, eventually reaching the dental pulp and causing infection.
Dental Trauma: Physical trauma to the tooth, such as a severe blow or injury, can damage the dental pulp. This trauma can result from accidents, falls, sports-related injuries, or any impact that affects the tooth’s structure.
Cracked or Fractured Tooth: A cracked or fractured tooth can expose the dental pulp to bacteria and lead to infection. Cracks can occur due to biting on hard objects, teeth grinding (bruxism), or weakened tooth structure from previous dental procedures.
Deep Dental Fillings: Large or deep dental fillings may irritate the dental pulp and cause inflammation or infection over time. It occurs when the filling is close to the pulp or if the pulp becomes exposed during the filling procedure.
Dental Procedure: Repeated dental treatment on a particular tooth, such as multiple fillings or extensive restorations, can eventually compromise the tooth pulp and necessitate root canal treatment.
Gum Disease: Advanced gum disease, also known as periodontitis, can lead to the formation of deep gum pockets and bacterial infection that can extend into the tooth’s root canals. In this case, the affected tooth may require root canal treatment. However, it’s important to note that not all cases of gum disease will require root canal treatment.
Dental Abscess: A dental abscess is a collection of pus usually caused by a bacterial infection. If left untreated, the infection may spread to the tooth pulp, leading to root canal problems.
Genetic Factors: Some individuals may be genetically predisposed to weaker tooth enamel or a higher risk of tooth decay, which can increase the likelihood of root canal issues.
It’s important to note that while these factors contribute to root canal problems, maintaining good oral hygiene practices, regular dental check-ups, and timely treatment of dental issues can help reduce the risk of developing root canal problems.
Root Canal Procedure
Root canal procedure, also known as endodontic treatment, can be performed by a general dentist or a specialist called an endodontist. It involves removing infected or damaged tooth pulp from the tooth root canal system.
Here is an overview of the root canal treatment process:
Preparing for Endodontic Treatment
Before the root canal treatments, the endodontist will typically examine the tooth and may take dental X-rays to assess the extent of the infection or damage and to determine any signs of inflammation or infection in the tooth surrounding bone.
Anaesthesia and Pain Management
Local anaesthesia is administered to numb the tissues surrounding the tooth root and ensure patient comfort during the procedure. A rubber dam, a thin sheet of latex or non-latex material, is placed around the tooth to isolate it and keep it dry during the treatment.
Accessing the Tooth’s Pulp Chamber
The endodontist creates a small access opening in the tooth’s crown to reach the pulp chamber. That is done using dental drills and specialised instruments. The infected pulp or infected nerve tissue will be removed.
Cleaning and Shaping the Root Canals
The endodontist carefully cleans and shapes the root canals using small, fine instruments called root canal files.
Irrigation and Medication
The root canals are irrigated with antimicrobial solutions to eliminate any remaining bacteria during the cleaning process. The endodontist may also place medication inside the canals to eliminate residual infection and promote healing.
Filling and Sealing the Canals
Once the canals are cleaned and shaped, they are filled with a biocompatible material called gutta-percha, a root canal filling material. It is a commonly used material in endodontic treatment, specifically for filling and sealing the root canal space after removing infected or damaged pulp.
Gutta-percha is a rubber-like material that fills the empty space and seals the canals, preventing recontamination. Sometimes, a temporary filling may be placed on top of the gutta-percha until the final restoration, such as a dental crown, is placed.
Post-Treatment Care Instructions
After root canal therapy, it is essential to follow proper post-treatment care instructions to promote healing and maintain the health of the treated tooth.
Here are some key guidelines to consider:
Oral Hygiene: Practice good oral hygiene by brushing your teeth twice daily and flossing daily. Use a soft-bristled toothbrush and be gentle around the treated tooth to avoid causing any discomfort or damage.
Avoid Chewing on Hard Foods: Avoid chewing on hard or sticky foods that can potentially damage the restored tooth or dislodge the temporary filling. Opt for softer foods and gradually reintroduce harder foods as advised by your dentist.
Take Prescribed Medication: If your endodontist has prescribed any pain medication or antibiotics, take them as directed. Follow the prescribed dosage and complete the entire course of medication to ensure effective healing and prevent potential infections.
Attend Follow-up Appointments: Attending all scheduled follow-up appointments with your dentist or endodontist is crucial. These appointments allow them to monitor the healing progress, remove the temporary filling if necessary, and determine the need for further treatment or the placement of a permanent restoration, such as a dental crown.
Report Persistent Discomfort: It is normal to experience some mild discomfort or sensitivity after a root canal procedure. However, contact your dentist immediately if you experience persistent or severe pain, swelling, or unusual symptoms. These could be signs of complications that require further evaluation and treatment.
Potential Complications and Risks
While root canal treatment is generally safe and successful, there may be potential complications and risks associated with the procedure.
These can include:
Incomplete Removal of Infected Material: In rare cases, some infected material may be left behind in the root canal system. That can lead to persistent infection or the need for further treatment.
Fractured Tooth: In some instances, the endodontically treated teeth may develop a crack or fracture, especially if it was already weakened before the root canal procedure. A fractured tooth may require additional treatment, such as a dental crown or even extraction if the damage is severe.
Reinfection: Although uncommon, a previously root canal treated tooth can become reinfected if bacteria enter the tooth’s root canal system. That can occur due to a defective restoration, new decay, or inadequate sealing of the canals during the initial treatment.
Discomfort or Sensitivity: Some patients may experience mild discomfort or sensitivity in the treated tooth, especially during the initial healing period. It is usually temporary and can be managed with over-the-counter pain relievers or as prescribed by your dentist.
Nerve Damage: Although rare, nerve damage can occur during the root canal procedure, leading to altered sensation or numbness in the affected tooth or surrounding tissues. That typically resolves over time, but you must notify your dentist if you experience any persistent or concerning symptoms.
Frequently Asked Questions About Root Canals
Is a root canal painful?
Root canal treatment is typically not painful. Before the procedure, the general dentist or endodontist will administer a local anaesthetic to numb the tooth and surrounding area, ensuring you are comfortable throughout the treatment. After the procedure, you may experience mild soreness or discomfort, but this can be managed with over-the-counter pain medication.
How long does a root canal procedure typically take?
The duration of a root canal procedure depends on various factors, such as the complexity of the tooth’s anatomy and the extent of the tooth infection. Generally, endodontic therapy can be completed in one to two appointments, each lasting about 60 to 90 minutes. However, additional visits may be required for retreatment or to place a dental crown over the root canal treated teeth in some cases.
What is the success rate of root canal treatment?
Root canal treatment has a high success rate, with studies indicating success rates of 85% to 95% for initial treatments. The long-term success of the treatment depends on several factors, including proper restoration of the tooth with a dental crown or filling, good oral hygiene practices, and regular dental check-ups. Sometimes, a root canal-treated tooth may require endodontic retreatment if new infections or complications arise.
Can a tooth that has had root canal treatments become infected again?
While it is rare for a tooth that has undergone root canal treatment to become reinfected, it is possible under certain circumstances. That can occur if there is a breakdown in the dental restoration, new decay develops, or the treated tooth is exposed to trauma. Regular dental check-ups and good oral hygiene are crucial in preventing reinfection and ensuring the long-term success of the root canal-treated tooth.
Are there any alternatives to root canal treatment?
The main alternative to root canal treatment is tooth extraction. However, saving the natural tooth whenever possible is generally recommended, as it helps maintain proper chewing function and prevents other oral health issues. Tooth extraction may require additional treatments such as dental implants, bridges, or dentures to restore the missing tooth, which can be more expensive and time-consuming than endodontic treatment.
How much does a root canal treatment cost?
The cost of a molar root canal treatment in Perth, Australia, can vary depending on several factors, including the dental clinic, the case’s complexity, the dentist’s experience, and any additional procedures or materials required. Generally, root canal treatment for a molar tooth can be more expensive than treatment for a front tooth due to the complexity of the procedure.
In Perth, the cost of a molar root canal treatment can range from approximately AUD 1,000 to AUD 2,500 or more. This cost typically includes the consultation, X-rays, the root canal procedure itself, and the placement of a temporary filling. However, it’s important to note that this is an estimated range, and the actual cost may vary.
It is important to consult with your dentist or endodontist to get an accurate cost estimate based on your specific situation.
Does dental insurance cover root canal treatment?
Dental insurance coverage for root canal treatment varies depending on the specific insurance plan. In many cases, dental insurance will provide partial coverage for the procedure. Reviewing your dental insurance policy or contacting your insurance provider to understand the extent of coverage for root canal treatment is recommended.
How soon can I eat or drink after a root canal procedure?
After root canal procedures, it is advisable to wait until the numbness from the local anaesthetic wears off before eating or drinking. That typically takes a few hours. It is recommended to start with soft foods initially and gradually transition to your regular diet as you feel comfortable. It is essential to avoid biting or chewing with the endodontically treated teeth until the final restoration, such as a dental crown, is placed to protect the tooth from further damage.
Does the root canal treatment work?
Despite having a relatively high success rate, you cannot always expect a happy ending for the endodontic treatment.
Here are some common complications which eventually will lead to root canal failure.
One potential complication is the failure to locate and treat all the canals associated with the infected tooth. Some teeth, especially molars, can have multiple canals. If any of these canals are missed during the treatment, it can lead to persistent infection and eventual root canal failure.
Another factor contributing to root canal failure is incomplete or inadequate cleaning and sealing of the canals. If the dentist does not thoroughly clean and disinfect the canals or properly seal them, there may be space left for bacterial growth, leading to reinfection and treatment failure.
Additionally, delaying root canal therapy can allow the infection to progress, potentially making the tooth weaker and more difficult to treat. In such cases, the tooth may become too compromised for successful treatment, and extraction may be necessary.
It’s important to remember that these complications are typically uncommon, and root canal treatment has a high success rate. Most cases are effectively treated, and the tooth can be saved. Dentists strive to provide thorough and successful root canal treatments, but inherent complexities and variations in individual cases can affect outcomes.
If you witness the symptoms below after the root canal treatment, contact our dentists for a consultation.
Pain or tenderness
Swelling
Discharge from the surrounding teeth
Sensitivity to heat or cold
Take the First Step Towards Your Perfect Smile!
Transform your smile and boost your confidence at Acts Dental! Our dedicated team of dental professionals is here to provide exceptional care and a personalised experience. We’re committed to delivering outstanding results with state-of-the-art technology and a range of services, including routine cleanings, cosmetic dentistry, and orthodontics. Experience our patient-centred approach, friendly atmosphere, and flexible payment options. Take the first step towards a healthier, more beautiful smile – schedule an appointment at Acts Dental today! Here’s our phone number (08) 9474 5083.
